
Biology and Impact of Mosquitoes in Montana
Mosquitoes are serious nuisance pests due to their persistent biting behavior and are responsible for affecting the health and well-being of humans, companion animals, livestock and wildlife. This MontGuide describes the biology and life cycle of mosquitoes, their impact in the state, and provides information on repellents and their proper use for personal protection.
Last Updated: 01/18by Marni Rolston, MSU, Entomology Research Associate, and Greg Johnson, Professor Emeritus of Veterinary Entomology
MOSQUITOES ARE A GROUP OF FLIES THAT OCCUR
in almost every region of every continent in the world except Antarctica. There are 3,200 recognized species worldwide with approximately 51 species found in Montana (Rolston et al. 2016). Mosquitoes are the most important arthropod affecting human health due to annoyance, discomfort from bites and transmission of diseases. They are second to ticks in affecting the health and well-being of livestock and companion animals. Lewis and Clark and the Corps of Discovery encountered enormous numbers of mosquitoes while traveling along the Missouri River in 1805. The expedition noted the mosquitoes were so intense they had to move their campsite to escape the relentless blood-sucking attacks. Their only other defenses were smoky fires and a repellent made from tallow and hog's lard.
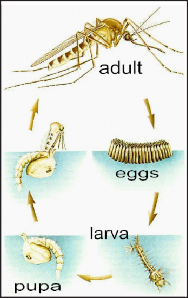
FIGURE 1. Mosquito life cycle showing the four different life stages: egg, larva, pupa and adult.
Description and Life Cycle
Mosquitoes can be classified as either floodwater or standing-water species. Floodwater mosquitoes (Ochlerotatus and Aedes species) deposit individual eggs during the summer on damp soil in low-lying areas. These eggs will hatch the following summer if the area is sufficiently flooded with runoff from snowmelt, rainfall or irrigation water. Because hatching and immature development are synchronized by flooding events, adults tend to emerge at the same time. The number of generations of floodwater mosquitoes produced in one summer depends on the number of times an area is flooded.
Standing-water mosquitoes (Culex, Culiseta and Anopheles species) overwinter as adults in animal burrows, inside buildings, under bridges, in culverts, etc. In late spring they come out of hibernation and begin depositing eggs on the surface of permanent or temporary pools of water. The eggs adhere to one another and collectively form a "raft" that floats on the surface of the water. Larvae hatch after a 24- to 48-hour incubation period. Adult populations of these mosquitoes gradually build-up through mid- summer, when their numbers peak.
The larvae of both floodwater and standing-water species are aquatic and must have non-moving water to complete development. Left undisturbed, they spend most of their time at the water's surface, feeding on algae and organic debris. They are often called wigglers because of their wiggling motion as they dive below the surface when disturbed. As they grow, mosquito larvae shed their skin, or molt, four times and then pupate. The pupal stage, a brief non-feeding stage during which the adult mosquito forms inside the larval skin, is also aquatic. Pupae are quite active and are often referred to as tumblers, describing their movement when disturbed. Development from egg to adult takes from 7 to 14 days in the summer (Figure 1).
The adult mosquito is a slender, delicate insect characterized by long legs, narrow, elongate wings and a proboscis that extends prominently from its head (Figure 1). Its entire body is covered in scales, and the various patterns and colors of these scales are important in identifying individuals to species. Shortly after emergence, both male and female mosquitoes feed on floral nectar for fluids and energy. After mating, females search for a suitable animal to bite and obtain a blood meal that is used for the development of eggs.
Many species of mosquitoes exhibit a feeding preference for certain animals while others have a wide host range. For example, the floodwater species Aedes vexans prefers large animals (cattle, deer and horses) and rarely feed on birds. In a 2006 study at Medicine Lake National Wildlife Refuge in northeast Montana, blood-fed mosquitoes were collected in traps and the animal from which the blood was taken was identified using a molecular test. Ae. vexans showed a preference for deer with 51 of 63 mosquitoes ingesting deer blood and 11 feeding on cattle. Similarly, Culiseta inornata demonstrated a marked preference for biting cattle with 26 of 32 specimens containing cattle blood. These species are serious nuisance pests of livestock, companion animals, and humans. They are not considered significant vectors (transmitters of disease) in Montana because they rarely feed on birds, which are the source for many mosquito-transmitted diseases.
Standing-water mosquitoes, such as Culex tarsalis and Culex pipiens, are less discriminate and will readily feed on many species of birds and mammals. These species are primary vectors of West Nile virus and other encephalitic viruses because they have more opportunities to pick up the virus by feeding on infected birds. In the Medicine Lake study, of the 63 blood-fed Cx. tarsalis collected, 46 fed on birds including Canada goose, cliff swallow, great horned owl, horned lark, mourning dove, ring-necked pheasant, sharp-tailed grouse, and western meadowlark, 12 fed on deer and five on cattle.
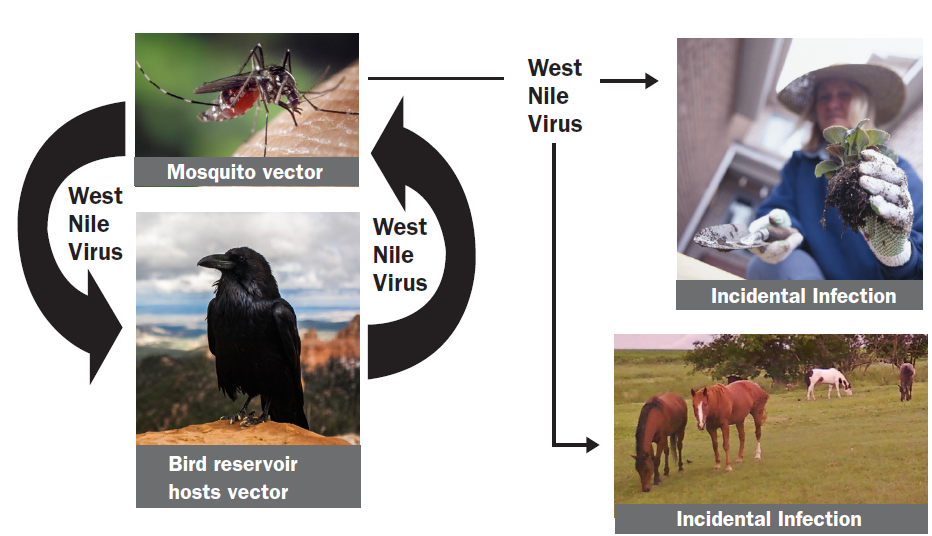
FIGURE 2. West Nile virus transmission cycle.
Impact of Mosquitoes
Mosquitoes do have an ecological value in serving as food for other organisms. However, this benefit tends to be overshadowed by the intense irritation they cause for livestock, wildlife and humans. Cattle attacked by mosquitoes often bunch together or constantly move to get relief from the intense biting. Disruption of normal grazing and resting behavior by mosquito swarms often results in reduced productivity in terms of decreased weight gains and milk production. For people, outdoor activities in the summer are often disrupted or even canceled because of the annoyance from swarming, biting mosquitoes.
Although mosquitoes can be a severe nuisance, the real danger they pose is disease transmission. In Montana, there are several encephalitic viruses and one nematode they can transmit. Fortunately, the frequency of transmission for most of these pathogens is low, and generally presents little risk of infection to humans or animals. The key exception is West Nile virus, which has become established in the state and is a health threat to humans, companion animals and wildlife.
West Nile Virus (WNV)
The first report of WNV in the U.S. was in New York City in 1999. It is unknown how the virus was introduced to the U.S., although it may have been from shipments of exotic birds or infected mosquitoes transported in ships or planes from overseas. The â??enzooticâ?? (animal cycle) of this virus involves various species of birds and mosquitoes (Figure 2). Certain birds play an important role in the amplification of the virus in the environment. These â??amplifying hostsâ?? develop high concentrations of virus in their bodies, making them a source of disease for feeding mosquitoes. Important amplifying hosts include crows, jays, robins and other passerine (perching) birds. In Montana and surrounding states, American white pelicans have also been identified as amplifying hosts.
The primary mosquito vector of WNV in Montana is Culex tarsalis. This species overwinters in Montana as an adult, and WNV may also successfully overwinter within the body of the mosquito (Nelms et al. 2013, Anderson et al. 2012). It is also hypothesized that WNV is reintroduced into the region each year by migrating birds. As the number of infected mosquitoes increases during the summer, the chance that they will feed and transmit WNV to other animals, including horses and humans, is increased. Humans and horses infected with WNV are not virus sources for blood feeding mosquitoes because the concentration of virus circulating in the blood of infected humans and horses is not high enough to infect a feeding mosquito. However, these low concentrations are still sufficient to trigger disease in affected individuals.
For people infected with WNV, 80 percent will develop no symptoms. The remaining 20 percent may develop West Nile Fever, characterized primarily by fever, headache, tiredness and body aches, and less than one percent may develop West Nile Neuroinvasive Disease, a severe form of WNV with symptoms including headache, high fever, neck stiffness, stupor, disorientation, coma, tremors, convulsions, muscle weakness, and paralysis. Approximately 500 people in Montana have been diagnosed with WNV fever or neuroinvasive disease since the disease was first reported in the state in 2002. Most of these cases occurred east of the Continental Divide in 2003 and 2007. There is no vaccine available for humans, so protection entails avoiding mosquito-infested areas, scheduling outdoor events when mosquitoes are less active, applying mosquito repellent, and wearing long-sleeved shirts and long pants.
Horses are very susceptible to WNV. In the fall of 2002 and summer of 2003, prior to the development of a WNV vaccine for equines, several hundred horses were infected with WNV in Montana; approximately 40 percent of these cases were fatal. Most of these cases occurred east of the Continental Divide. The number of cases dropped dramatically following the release of a vaccine that provides protection for equines when administered about six weeks before the mosquito season begins. Sometimes booster vaccinations are recommended later in the season, depending on the potential for future virus exposure.
Other mosquito-transmitted viruses have been reported in the state, although their frequency of transmission is very low. These include Western equine encephalitis, last reported in Montana in 1995; St. Louis encephalitis, with two reported human cases in Montana since 1964; and La Crosse encephalitis, with one reported human case from Montana since 1964. These diseases have cycles similar to WNV in that passerine birds are amplifying hosts and transmission occurs in late summer following a build-up of infected mosquitoes. Why these diseases are not more prevalent is unknown.
Canine Heartworm
Canine heartworm is a nematode that lives in blood vessels of the heart and lungs of dogs and other canines, including foxes and coyotes. Cats can also become infected. Adult nematodes release larvae, called microfilaria, into the dog's bloodstream where a mosquito may ingest them when feeding on blood. The larvae develop into an infective stage in the mosquito; this requires several weeks depending on temperature. The larvae migrate to the mosquitoâ??s head and, when the mosquito feeds on a dog, they crawl down the mosquitoâ??s mouthparts and into the feeding wound where they enter the blood stream. After several months, the heartworm larvae enter the venous circulation and become established in the right ventricle of the heart and pulmonary arteries. Upon maturation, the female nematodes begin releasing microfilariae. A feeding mosquito ingests the microfilariae to complete the cycle.
The risk of transmission for canine heartworm is low in Montana due to the cool, short summers, which prevent the microfilaria from developing to the infective stage in the mosquito. A three-year heartworm survey was conducted in Montana where 3,490 canine blood samples were tested and found 24 positive with only two of these from dogs that had no out-of-state travel history. To assess the prevalence of heartworm infection in mosquitoes in Montana, over 60,000 mosquitoes were collected from 12 Montana counties in 2005 and 2007 and tested for the parasite. None of the mosquitoes tested positive for canine heartworm.
Even though the risk of heartworm transmission in the state is low, it is strongly recommended that pet owners contact their veterinarian for information regarding preventive treatments to control heartworm microfilaria. Treatment of adult nematodes is difficult and complicated, but controlling microfilariae is simple, only requiring a chewable tablet containing a nematicide once a month.
Personal Protection
There are many products available that provide protection from mosquitoes. The Center for Disease Control (CDC) recommends four over-the-counter products containing active ingredients registered by the Environmental Protection Agency (EPA) for use on skin and clothing. These include DEET, Picaridin, Oil of Lemon Eucalyptus, and IR3535. The EPA characterizes the active ingredients in DEET and Picaridin as "conventional repellents" and the active ingredient of Oil of Lemon Eucalyptus (not an essential oil) and IR3535 as "biopesticide repellents," which are derived from natural materials. Additional information on these repellents can be found at http://www.cdc.gov/ncidod/dvbid/westnile/RepellentUpdates.htm.
There have been very few documented cases of toxicity from DEET products over the past 50 years, and the CDC determined in 1998 that its "normal use does not present a health concern to the general U.S. population." However, it can be harmful if used inappropriately; therefore it is important to apply it in a conservative, common-sense manner. DEET (trade names OFF!, Repel, Bens, Sawyer, Coleman and others) is available in concentrations ranging from four percent to 100 percent, with the lower concentrations providing approximately 1½ to 2 hours of protection and a 24 percent concentration providing an average of five hours of protection. Using products with concentrations higher than 50 percent does not increase the length of protection. When applying DEET on children, use low-concentration products, and never use it on infants younger than two months of age.
Picaridin had been used in Europe, Australia, Asia and Latin America for many years before it was approved for use in the U.S. in 2005. In the U.S. it is sold under various trade names, such as OFF!, Cutter, Sawyer, Avon, REPEL, Natrapel and Centaura. Its effectiveness is comparable with similar concentrations of DEET and it is considered slightly less toxic.
Oil of Lemon Eucalyptus (trade names REPEL, Cutter, Coleman and OFF!) was also approved for use in 2005. It provides protection similar to low concentration DEET products. However, it should not be used on children younger than three years old.
The repellent IR3535 has been added to Avona's Skin-So-Soft lotions and is now sold as Skin-So-Soft Bug Guard. Conflicting data exist about the efficacy of IR3535 to repel mosquitoes; a USDA study determined a 25 percent concentration of IR3535 offered 1⁄10 to 1⁄100 the protection against biting mosquitoes as a 25 percent DEET product, while another study found protection times of up to 10 hours. It has been used in Europe for 20 years with few adverse effects before it was approved for use in the U.S. in 1999.
Natural and plant-based compounds such as vanilla extract, banana oil, aromatic oils, and vitamin B-1 have shown little efficacy in repelling mosquitoes, and those that do need to be reapplied continuously.
Certain precautions should be considered when applying any insect repellent. They should only be applied on exposed skin and/or clothing, and should never be used on cuts, wounds, eyes or near the mouth. When applying to the face, repellents should first be sprayed on the hands and then spread onto the face. The same procedure can be followed when using a repellent on children. After returning indoors, wash skin treated with insect repellent with soap and water, and wash treated clothing before wearing it again.
Typically, a thin film of repellent is effective; however, more may be applied if biting insects don't respond to the first application. In general, the more active ingredient a repellent contains, the longer it protects against mosquito bites. Protection also varies depending on conditions such as temperature, rate of perspiration, and exposure to water.
Products containing permethrin, an insecticide and repellent, are available for use on clothing, shoes, bed nets and camping gear. Permethrin-treated clothing can be washed repeatedly, but the insecticide must be reapplied occasionally. Some commercial products are also available pretreated with permethrin.
Other preventive measures can be taken to protect against mosquito bites when outdoors. Be aware of peak biting times at dawn, dusk, and early evening. Schedule outdoor activities to avoid these times, and wear long- sleeved shirts and long pants.
References
Carroll, S.P. 2008. Prolonged efficacy of IR3535 repellents against mosquitoes and blacklegged ticks in North America. Journal Medical Entomology. 45(4): 706-14.
Dougherty, R., G. Johnson, S. Alvey, and G. Hokit. A survey of Montana mosquitoes for canine heartworm, Dirofilaria immitis, and development of an infection risk model. (in prep).
Fradin, M.S., and J.F. Day. 2002. Comparative efficacy of insect repellents against mosquito bites. New England Journal of Medicine. 347(11): 13-18.
Hale, K. 2007. Investigations of the West Nile virus transmission cycle at Medicine Lake National Wildlife refuge, Montana, 2005 - 2006. Montana State University, M.S. thesis. 74 p.
Johnson, G., N. Nemeth, K. Hale, N. Lindsey, N. Panella, and N. Komar. 2010. Surveillance for West Nile Virus in American White Pelicans, Montana, USA, 2006 - 2007. Emerging Infectious Diseases. 16: 406 - 411.
Knapp, S., M. Rognlie, and L. Stackhouse. 1993. Range of heartworm (Dirofilaria immitis) infection in Montana dogs. Journal of Parasitology. 79: 618-620.
Nelms, B., E. Fechter-Leggett, B. Carroll, P. Macedo, S. Kluh, and W. Reisen. 2013. Experimental and natural vertical transmission of West Nile virus by California Culex (Diptera: Culicidae) mosquitoes. Journal of Medical Entomology. 50(2):371-378.
Rolston, M., G. Johnson, and G. Hokit. 2016. A Taxonomic Checklist of the Mosquitoes of Montana With Notes On New Geographic Distributions. Journal of the American Mosquito Control Association. 32(4):326-328.
Scoles, G.A. 1999. Vectors of canine heartworm in the United States: A review of the literature including new data from Indiana, Florida, and Louisiana. In Recent Advances in Heartworm Disease: Symposium 1998. M.D. Soll and D.H. Knight, eds. American Heartworm Society, Batavia, Illinois.

